India one of the worst places to die, UK best says new report
A new report on Global palliative care has named India as the worst places to die and Britain the best, but singles out Kerala as a ‘beacon of hope’ for being the only Indian state to have a formal policy on palliative care services.
A new report on global palliative care has named India as one of the worst places to die and Britain the best, but singles out Kerala as a ‘beacon of hope’ for being the only Indian state to have a formal policy on palliative care services.
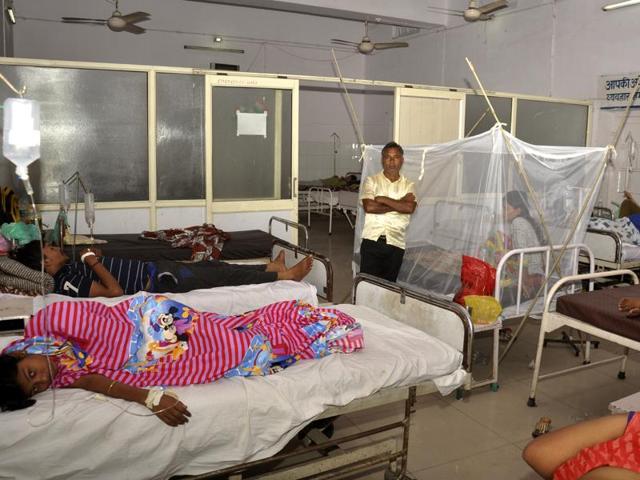
The report from the Economic Intelligence Unit, titled ‘The quality of death: Ranking end-of-life care across the world’, ranks India at number 40 in its ‘Quality of Death Index’ that measures the current environment for end-of-life care services in 40 countries.
The report says that with the exception of Kerala, India has little government funding for end-of-life care, and quotes MR Rajagopal of Pallium India as saying: “In India less than 1% is spent on healthcare so it’s not only palliative care that suffers. There is no public funding, there is no socialised medicine and the same holds true for palliative care.”
In a detailed case study on Kerala, the report says: “While India ranks at the bottom of the Index in overall score, and performs badly on many indicators, Kerala, if measured on the same points, would buck the trend. With only 3% of India’s population, the tiny state provides two-thirds of India’s palliative care services”.
The state’s palliative care system, the report says, is being studied by experts from across the world for its “potent combination of government support and civic involvement in end-of-life care”.

The report says: “Kerala’s unique system proves the importance of these points, embodied in the Neighbourhood Network in Palliative Care (NNPC) project. Since 2001 this project, which grew from a more traditional, institutional-based palliative care experiment, has employed an army of volunteers that deliver services to patients who largely remain in their own homes”.

“The system is community run and operated and is funded largely through local micro-donations of as little as Rs 10 (21 US cents) per month—although in recent years local and regional governments have becoming increasingly involved as the project has gained prominence”.
The NNPC’s volunteers do not provide medical services, but identify those in their community who need care and supplement the work of healthcare professionals linked to the state’s 230 local palliative care units.
The report says: “Importantly, after a few days’ theoretical and practical training, the volunteers can provide psychological, social and spiritual support. It is this that marks the NNPC out from more medical-oriented—and expensive—systems in use elsewhere”.
The report make several recommendations to improve palliative care across the world.
Get Current Updates on India News, Lok Sabha Election 2024 live, Infosys Q4 Results Live, Elections 2024, Election 2024 Date along with Latest News and Top Headlines from India and around the world.




