Navigating the vaccine challenge
Getting the product, quantity, condition, place, time and cost right is key
For anyone seeking to understand the path ahead for vaccines and vaccination for Sars-CoV-2, there is abundant confusion. Part of this is because there is divergence in information from official sources, academics and “unofficial” sources, and a difference in opinion on the timeliness and completeness.
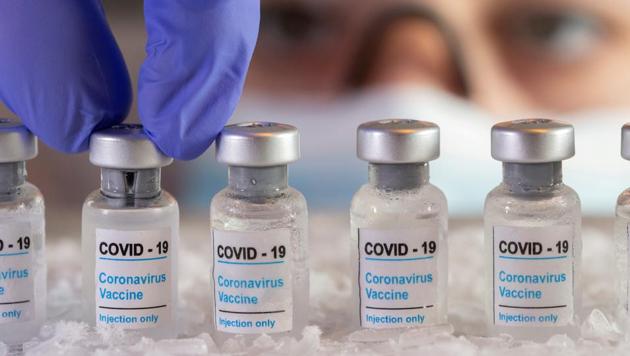
Press releases tell us that vaccines are performing well. On December 2, the United Kingdom (UK)’s Medicines and Healthcare Products Regulatory Agency became the first regulator to grant temporary authorisation based on a phase III trial, to Pfizer and BioNTech’s mRNA-based Covid-19 vaccine. On December 7, the UK began the process of administering vaccines.
Results from the Astra-Zeneca/University of Oxford vaccine, based on a chimpanzee adenoviral vector, well exceed the 50% efficacy requested by the World Health Organization (WHO) and regulators, leading to the reasonable assumption that most vaccines that are based on the spike protein of Sars-CoV-2 will be successful.
In India, Pfizer has applied to the Central Drugs Standards Control Organisation for emergency approval, under the provisions of the New Drugs and Clinical Trials Rule, 2019, which allow the national regulatory authority to waive clinical trials. Even if Pfizer is granted approval, it is unlikely that this will be a vaccine that can be widely deployed because it requires storage at -70 degrees Celsius. Given the limited capacity of even cold storage at -20 degrees Celsius as required by the Moderna vaccine, it is likely that India’s national immunisation system, and those of other low- and middle-income countries, will opt for vaccines that can be stored at the more widely available facilities that hold vaccines at 2-8 degrees Celsius.
If vaccines that will not be used for national immunisation programmes are given limited or full approval, the ability to purchase vaccines will differentiate sections of society between those with purchased access and those who must wait for the government to provide vaccines. This situation already exists for many vaccines, such as influenza or chickenpox where vaccines are available in the private sector. Open and transparent discussions about the role of the private sector and access to vaccines are essential for a clearer picture of what lies ahead.
In terms of production capacity, figures vary, but a survey of 113 manufacturers by the Coalition for Epidemic Preparedness Innovations and partners between March and June 2020 estimated that global capacity was two to four billion doses by the end of 2021. Vaccine production landscapes tend to be slow to change, but much more optimistic figures are now being projected, with the Duke Global Health Innovation Center stating that purchase of more than nine billion doses is in discussion and India alone already has an advance market commitment of 1.6 billion doses. This figure does not align with the government’s announcement of financial commitments to vaccines or plans for immunisation, and company announcements of their production capacity and commitment not just to India, but to global supply through the COVAX facility.
Even if the figures are correct, and India will have access to 1.6 billion doses of vaccines by the end of 2021, there are significant challenges to getting these doses to where they are needed. The WHO has six rights of supply-chain management for immunisation, which are right product, right quantity, right condition, right place, right time and right cost. Making sure that all of these logistics are in place requires permutations of product packed volume, temperature for transport and storage, location of supply and delivery, cycle for vaccination and restocking. Availability of refrigerated transport, security of transport, opportunities for pilferage and replacement with fake products are all very real concerns for which preparation is necessary.
To accompany the complexity of storage and supply, which in India will be managed by the National Cold Chain Vaccine Management Resource Centre and the electronic Vaccine Information Network, redeveloped as COVIN, we will need to train vaccinators, have additional supplies needed for immunisations, prepare for immunisation sessions and establish systems for waste disposal. And all that, as we develop and use methods to identify and track individuals who need the vaccine.
India does not have an adult immunisation programme beyond the tetanus/diphtheria vaccination for pregnant women. Hence, in the prioritisation lists that have been announced, identifying and reaching all priority groups will be a challenge. States have been asked to list public and private health care workers, and this is feasible and being done.
However, moving beyond health care workers and other essential workers, however defined, to the elderly and those with co-morbidities as indicated in official announcements will be difficult and there is a need to prepare for falsified documents and fraud.
As important as the issue of delivering vaccines to those prioritised, and not those who try to beat the system is the global concern for migrants and refugees who might be excluded from vaccination based on lack of residency documentation. Ensuring that both doses of a two-dose schedule are delivered is also a challenge since drop-outs are already known to be an issue, particularly for the most vulnerable populations, for infant immunisation. This is likely to much greater with adult immunisation.
Not all problems can be anticipated, but we have experience with strengthening immunisation and with the conduct of campaigns, particularly in the last decade. While the government is using that experience to plan for a range of product, supply and logistic scenarios, sharing plans and developing the right partnerships is important, because in this enterprise, all of us are stakeholders.



