Will US Covid vaccine patent waiver lead to more jabs in India? Not really
Like many developing nations, India is struggling to cope with a surge in vaccine demand, amid a shortage, even as it battles the second wave of Covid-19 infections
Maya Johal, a 29-year-old schoolteacher in Delhi, booked herself for a coronavirus vaccine shot a week ago, but is still awaiting her turn. “I was turned away from a vaccine facility. I was told that supplies were over,” she said.
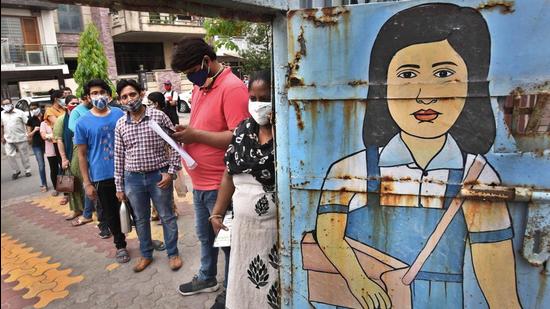
Like many developing nations, India is struggling to cope with a surge in vaccine demand, amid a shortage, even as it battles the second wave of Covid-19 infections.
The global inequity
Mass immunisation is the only way to end the pandemic but rising global inequality in vaccine access stands as a colossal hurdle. “Most developing countries will not have widespread access to the shots before 2023 at the earliest,” said a recent forecast by the Economist Intelligence Unit.
According to an April 26 assessment by the Global Commission for Post-Pandemic Policy, a United States (US)-based thinktank, the “declared (manufacturing) target” for approved vaccine doses is 14.6 billion by 2021-end. This requires 13.4 billion more doses to be produced during the next eight months, or an average of 1.675 billion doses per month. “That is four times the monthly run-rate seen in April,” it said.
According to WHO, nearly 80% of Covid-19 vaccines have been administered in just 10 rich countries, while more than 2.5 billion people await their first shots.
A surprising US decision on May 5 has however stirred hopes of bridging the great vaccine gap. The Joe Biden administration said it would support temporarily waiving intellectual property protections for coronavirus vaccines, something India and South Africa are pushing for.
If the proposal moved by India and South Africa jointly on October 2, 2020, at World Trade Organization (WTO) goes through with US backing, it would prevent countries from implementing patents, trade secrets or other monopolies on Covid-19 vaccines under the WTO’s agreement on Trade-Related Intellectual Property Rights or TRIPS.
Also Read | Will work with COVAX, partners to distribute 80mn Covid-19 vaccines: Prez Biden
India’s waiver application is, however, not limited to vaccines but includes “diagnostics and therapeutics in relation to prevention, containment or treatment of Covid-19”. Pharma companies enjoy patents, which legally protect their products from being copied or cheaper generic versions being made. This allows developers of original products a monopoly to earn profits, for 20 years at the minimum.
Decoding the jab
Analysts agree that the US stand marks a radical change of policy but are yet unsure whether this will achieve any real result for developing countries like India.
“Whether America’s support of the waiver will have impact on people’s lives in India depends on a number of factors, such as how quickly the negotiations move and what the terms of the final waiver are,” said Priti Radha Krishtel, co-founder of Initiative for Medicines, Access & Knowledge (I-MAK).
Experts say waiving patents, especially of vaccines based on the highly effective mRNA technologies, will be of little help in the short run. Most manufacturers will simply not have the know-how – which are technological processes not protected by patents – to produce quality and safe vaccines. Raw materials – nanolipids and bioreactor bags -- are already scarce.
“The EU is still opposed to the idea (of a waiver). Between Switzerland, Germany and Japan, there is a formidable opposition to even discuss the proposal (at WTO),” said Biswajit Dhar, an economist with the Jawaharlal Nehru University, who has previously advised the Union government on WTO deals.
Also Read | A new chapter for the TRIPS waiver proposal
WTO’s director general Ngozi Okonjo-Iweala has said the body would take up the issue of IP waiver for Covid vaccine in December.
“Just having access to a patent does not mean all countries are equipped with the technological infrastructure to scale up manufacturing of generic counterparts. Companies such as Moderna and Pfizer will need to establish helpful partnerships and collaborations with companies, say in India,” said Bhramar Mukherjee, professor of global public health at University of Michigan.
A web of licences
Developing countries also may not understand the full web of intellectual property rights governing a vaccine candidate.
“For example, the underlying technology used to develop a vaccine can be protected by patents, while manufacturing methods and techniques (know-how) can be protected by trade secrets,” wrote authors Mario Gaviria and Burcu Kilic in the first analysis of mNRA vaccine patents in the journal Nature published on May 12, 2021. According to them “multiple forms of intellectual property protection stand in the way of equitable access and fair allocation”.
Some of the most impressive mRNA-based vaccine candidates are produced by the likes of Moderna, Pfizer and BioNTech, CureVac and Arcturus.
In their paper, “A network analysis of Covid-19 mRNA vaccine patents”, Gaviria and Kilic explain that this vaccine platform uses multiple technologies, including the main mRNA technology, lipid nanoparticle technology and a delivery-system. A lipid nanoparticle, which is like a ball of fat, is used to deliver the mRNA to the cells, which “makes it a key aspect of the vaccine’s technology”, the authors write. After the mRNA is delivered to a cell, it “instructs the cell to produce the SARS-CoV-2 spike protein, thereby eliciting an immune response”. Each of these steps involves a sub-licence. The authors note that US federal filings “reveal a series of sub-licenses for mRNA-related patents that stem from the University of Pennsylvania to both Moderna and BioNTech”.
Analysis by Gaviria and Kilic also show that the University of Pennsylvania exclusively licensed their patents to “mRNA RiboTherapeutics”, a firm which then “sublicensed them to its affiliate CellScript”, another biotech firm. CellScript then sublicensed the patents to Moderna and BioNTech.
Also Read | Head of Canada’s Covid vaccine roll-out accused of misconduct; new chief named
Pointing to a complex web, the researchers noted: “However, the patent numbers are redacted in all the filings, making it difficult to determine which are relevant to the production of Covid-19 vaccines.”
India’s advantage and way forward
Health experts say one potential solution to end the vaccine shortage — one that the World Health Organization has backed — is a “patent pool” similar to one used to make HIV drugs available to poorer countries in the 1990s. It depends on voluntary sharing of recipes and data, for which no Covid-19 vaccine manufacturer has shown interest yet.
Trade experts such as JNU’s Dhar said sIndia has an indigenously developed vaccine candidate like Covaxin, manufactured by Bharat Biotech in collaboration with the state-run Indian Council of Medical Research and National Institute of Virology.
“Unless knowledge and expertise are also transferred, largescale manufacturing of vaccines may not be feasible,” executive director of Bharat Biotech Sai D. Prasad said, saying technology transfer partnerships are needed, aside from the main recipe for the vaccines.
Many public health professionals who advocate vaccines as a “global common good” say developing nations do have the capacities to make quality shots.
The Coalition for Epidemic Preparedness Innovations recently drew up a list of 250 companies globally capable of making quality vaccines if IP waiver is obtained. These include Bangladesh’s Incepta, India’s Bharat Biotech and South Africa’s Aspen Pharmacare.
Els Torreele, policy associate at the University College London’s Institute for Innovation and Public Purpose, said India, as a “large economy with abundant capacities for pharmaceutical production including vaccines, is in an excellent position to quickly retool production lines for the manufacturing of a variety of technologies and raw materials needed for the global scale up of Covid-19 vaccines”.
Continue reading with HT Premium Subscription





