Mohalla clinics a model for universal health coverage
The mohalla clinic at Sarai Kale Khan receives around 100 patients daily with complaints of fever, cough and cold, skin rashes, stomach upset, diabetes and hypertension.
Rajni Chauhan, 34, walked into the mohalla clinic in Sarai Kale Khan at 11 am to get treatment for a persistent itch on her right arm that wasn’t improving with skin ointments. She was prescribed a thyroid test at the clinic. The test was free, and after she was diagnosed with hypothyroidism, she was given free medicines. “This clinic is close to my home and the best part is there are no queues,” said Chauhan.

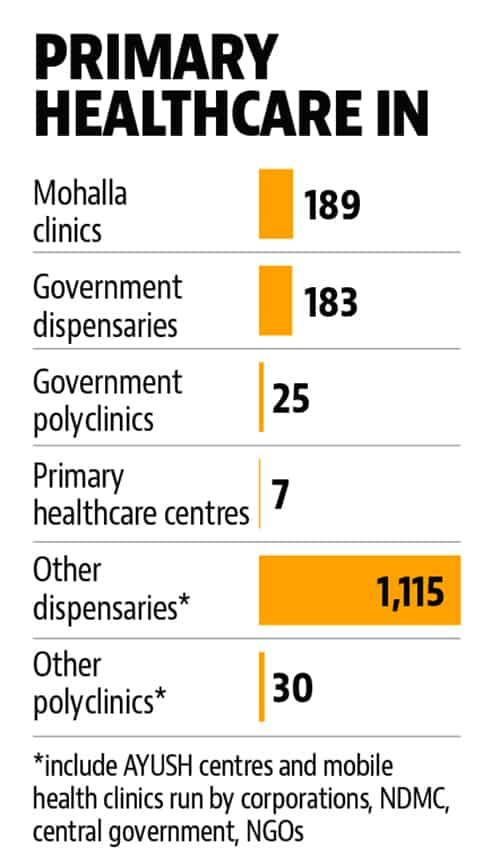
The mohalla clinic at Sarai Kale Khan receives around 100 patients daily with complaints of fever, cough and cold, skin rashes, stomach upset, diabetes and hypertension. Since the first clinic was set up in West Delhi’s Peera Garhi in July 2015, 189 more have come up. The target is to set up 1,000 clinics, one in every 5km radius.
States like Telangana, Karnataka and Andhra Pradesh are setting up urban health centres on the mohalla clinic model that is often run in portacabin clinics built at a cost of ₹20 lakh per two-room clinic, and provides consultation, 80 medicines and 212 tests free of cost. All the mohalla clinics are run by doctors hired on a contractual basis and paid ₹40 per patient as an incentive.
There is a shortfall of health workers, with pharmacists and auxilliary nurse midwives (ANM) being moved from hospitals and dispensaries to staff clinics. “A decision has been taken to hire additional pharmacists and ANMs on ad hoc basis after a test right after the model code of conduct is lifted,” said a senior official from Delhi government’s health department.
The clinics are run between 8 am and 2 pm on working days in Delhi, and till 4.30 pm in Karnataka. “The services are usually utilised by the urban poor, who are daily wage labourers, so evening clinics are essential... our urban clinics also provide speciality and general medicine consultation in the evenings between 5 pm and 8 pm,” said Dr Prabhudev D Gowda, nodal officer for National Urban Rural Health Mission (NURHM), Karnataka, which is setting up 364 mohalla clinics.
Andhra Pradesh, which has set up 244 urban primary health clinics in public-private partnership mode since October 2016, also offers specialist advice through telemedicine and evening clinics between 4 pm and 8 pm. “The clinics are open all 365 days, including Sundays and holidays... Our model is very different from the Delhi government’s and we provide more services,” said G Vasudev Rao, state programme officer NURHM, Andhra Pradesh.
One of the biggest drawbacks of Delhi’s mohalla clinics is that they do not offer ante-natal checkups, immunisation or basic emergency care. “If a patient comes to me with injuries, I do not have dressing material, I do not have tetanus shots, so I have to refer them to the hospital,” said a mohalla clinic doctor who did not want to be named.
There is also a shortage of free medicines for chronic diseases like diabetes, hypertension and thyroid.
Despite the shortcomings, former health secretary K Sujatha Rao feels it is a “superb” model. “It is low cost and extremely effective. Also, the clinics are located right where the people live. Given support from the government, they could be scaled up to provide effective, preventive healthcare services and immunisation. This is the way to go about universal health coverage,” she said.
Get Current Updates on India News, Ram Navami Live Updates , Lok Sabha Election 2024 live, Elections 2024, Election 2024 Date along with Latest News and Top Headlines from India and around the world.




